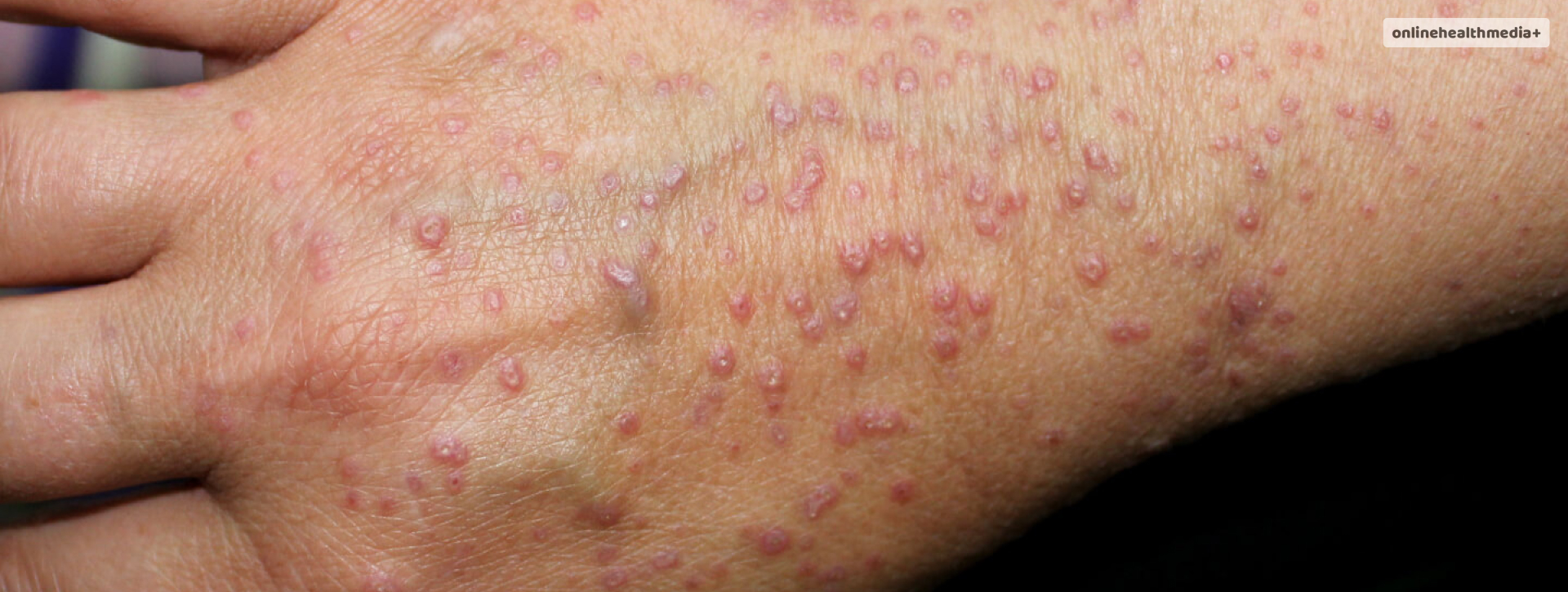
Exploring Lichen Planus Treatment Options : Lifestyle changes & More.
Lichen planus is a chronic inflammatory skin condition that can affect various parts of the body, including the skin, mucous membranes, nails, and scalp.
While the exact cause of lichen planus remains unclear, its impact on an individual’s quality of life can be significant.
Managing and treating this condition is crucial to alleviate symptoms and prevent complications.
In this article, we will delve into the various treatment options available for lichen planus, ranging from conventional medical approaches to alternative therapies.
Understanding Lichen Planus
Before discussing treatment options, it’s essential to have a basic understanding of lichen planus. This condition is characterized by the development of purplish, flat-topped bumps or lesions that can be itchy or painful. These lesions may appear on the skin, mucous membranes, or other affected areas.
The exact cause of lichen planus is not well-defined, but it is believed to involve an abnormal immune response.
Triggers such as certain medications, viral infections, and stress have been associated with the onset of lichen planus.
Additionally, genetic factors may contribute to an individual’s susceptibility to this condition.
Conventional Medical Treatments

1. Topical Corticosteroids:
One of the primary treatments for lichen planus involves the use of topical corticosteroids. These medications help reduce inflammation, itching, and discomfort associated with the lesions.
Topical corticosteroids are available in various strengths and formulations, and their application frequency depends on the severity of the condition.
2. Systemic Corticosteroids:
For more widespread or severe cases of lichen planus, oral corticosteroids may be prescribed. These medications work throughout the body to suppress the immune response and reduce inflammation.
However, long-term use of systemic corticosteroids can lead to side effects, so they are typically prescribed for a limited duration and under close medical supervision.
3. Immunosuppressive Drugs:
In cases where corticosteroids alone may not be sufficient, immunosuppressive drugs such as methotrexate or cyclosporine may be considered.
These medications work by suppressing the immune system, helping to control the abnormal immune response associated with lichen planus.
4. Retinoids:
Topical or oral retinoids, such as acitretin, may be prescribed to manage lichen planus. Retinoids are derivatives of vitamin A and can help regulate skin cell growth and reduce inflammation.
However, they also carry potential side effects and require careful monitoring.
5. Phototherapy:
Light therapy, or phototherapy, involves exposing the affected skin to ultraviolet (UV) light. This treatment can help reduce inflammation and itching associated with lichen planus lesions.
Phototherapy is often used in conjunction with other treatments and is typically administered under medical supervision.
Alternative and Complementary Therapies
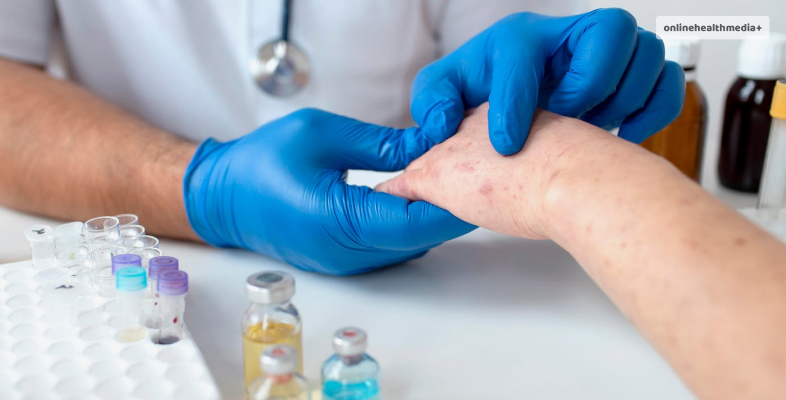
1. Topical Calcineurin Inhibitors:
Calcineurin inhibitors, such as tacrolimus and pimecrolimus, are topical medications that suppress the immune response and may be considered as an alternative to corticosteroids.
These medications are particularly useful for treating lichen planus in sensitive areas, such as the genitalia or face.
2. Herbal Remedies:
Some individuals explore herbal remedies and natural supplements as complementary treatments for lichen planus.
However, it’s crucial to approach herbal remedies with caution, as their efficacy and safety are not always well-established.
Aloe vera, chamomile, and tea tree oil are examples of herbs that some people find soothing for their lichen planus symptoms.
3. Diet and Lifestyle Modifications:
Maintaining a healthy lifestyle and making dietary changes may contribute to managing lichen planus symptoms.
Some individuals report improvements in their condition by adopting an anti-inflammatory diet, avoiding potential triggers, and managing stress through techniques such as meditation or yoga.
4. Homeopathic Treatments:
Homeopathy is another alternative approach that some individuals explore for lichen planus. Homeopathic remedies are selected based on the specific symptoms and characteristics of the individual.
However, scientific evidence supporting the efficacy of homeopathy for lichen planus is limited, and it’s essential to consult with a qualified healthcare professional before pursuing such treatments.
Comprehensive Treatment Guidelines for Lichen Planus
Medical Interventions
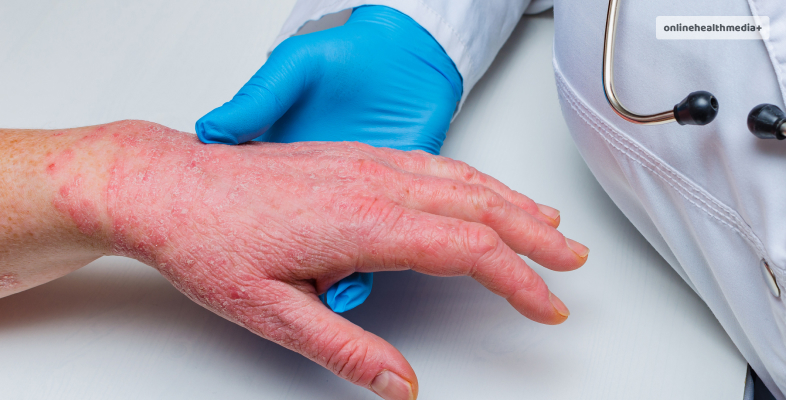
1. Topical Corticosteroids:
– Application Guidelines: Topical corticosteroids are the first line of treatment for localized lichen planus. Dermatologists may prescribe varying strengths based on the severity. Apply a thin layer to affected areas, following the prescribed frequency.
2. Systemic Corticosteroids:
– Considerations: In cases of widespread or severe lichen planus, oral corticosteroids may be prescribed. Due to potential side effects, they are typically used for short durations under close medical supervision.
3. Immunosuppressive Drugs:
– Usage: Methotrexate or cyclosporine may be considered in cases where corticosteroids alone are insufficient. These drugs suppress the immune response and are prescribed cautiously, given potential side effects.
4. Retinoids:
– Topical or Oral: Retinoids, such as acitretin, can regulate skin cell growth and reduce inflammation. Dermatologists may recommend topical or oral formulations based on the extent and location of lichen planus lesions.
5. Calcineurin Inhibitors:
– Alternative to Corticosteroids: Tacrolimus and pimecrolimus are topical calcineurin inhibitors that can be considered, especially in sensitive areas like the face or genitalia.
6. Phototherapy:
– UV Light Exposure: Controlled exposure to ultraviolet (UV) light, known as phototherapy, can aid in reducing inflammation. This is often employed in conjunction with other treatments.
Lifestyle Adjustments
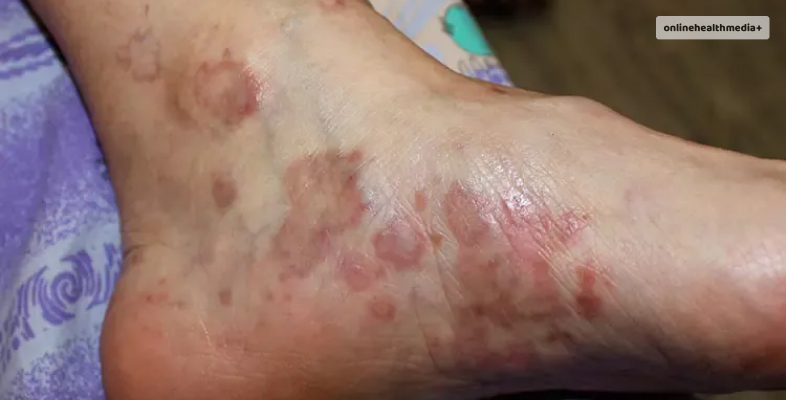
1. Skincare Practices:
– Gentle Cleansing: Use mild, fragrance-free cleansers to avoid skin irritation. Harsh products can exacerbate lichen planus symptoms.
2. Avoidance of Triggers:
– Identify and Eliminate: Determine and eliminate potential triggers such as certain medications, allergens, or stressors that may exacerbate lichen planus.
3. Stress Management:
– Mind-Body Techniques: Incorporate stress-reduction techniques, including meditation, yoga, or deep breathing exercises, to minimize the impact of stress on lichen planus.
4. Dietary Modifications:
– Anti-Inflammatory Diet: Consider adopting an anti-inflammatory diet rich in fruits, vegetables, and omega-3 fatty acids. Limit intake of processed foods, sugars, and potential allergens.
5. Hygiene Practices:
– Avoid Aggressive Scrubbing: Gentle hygiene practices, avoiding aggressive scrubbing or scratching, can prevent further irritation.
6. Clothing Choices:
– Breathable Fabrics: Choose loose-fitting, breathable fabrics to minimize friction and allow airflow, particularly in areas prone to lichen planus lesions.
Ongoing Monitoring and Follow-up
– Regular Dermatologist Visits: Periodic follow-up visits with a dermatologist are essential to monitor progress, adjust treatment plans, and address any emerging concerns.
– Communication with Healthcare Providers: Maintain open communication with healthcare providers to report any changes in symptoms, side effects from medications, or concerns about the treatment plan.
Conclusion
It’s crucial for individuals with lichen planus to work closely with healthcare professionals to determine the most appropriate treatment plan for their specific case.
Regular monitoring, follow-up appointments, and open communication with healthcare providers are essential for effective management of lichen planus and minimizing the impact of this chronic condition on a person’s daily life.
As research continues and our understanding of lichen planus improves, new and more targeted treatment options may emerge, offering hope for enhanced outcomes and improved quality of life for those affected by this challenging skin condition.
Also read
- Top Electric Toothbrush For Kids.
- The Most Common Types Of Bicycle Accident Injuries.
- Compelling Reasons To Incorporate Shilajit Into Your Diet.