What Is Frontotemporal Dementia? Answered: Definition, Types And More!
Note: The information in this article is not intended to substitute professional medical advice, diagnosis or treatment. All images and text presented are for general information purposes only. Contact your healthcare provider if any of the information is relatable.
Asking, “What is frontotemporal dementia?” Here’s your answer. Frontotemporal dementia (FTD) is a complex and progressive neurological disorder characterized by the degeneration of nerve cells in the frontal and temporal lobes of the brain. This leads to changes in behavior, personality, language, and executive function.
FTD is one of the less common types of dementia, accounting for approximately 10-15% of all cases, but it represents a significant burden for affected individuals and their families. A group of brain disorders that affect the temporal and frontal lobes of the brain.
Read till the end to know more about the 7 stages of frontotemporal dementia.
What is FTD Dementia?
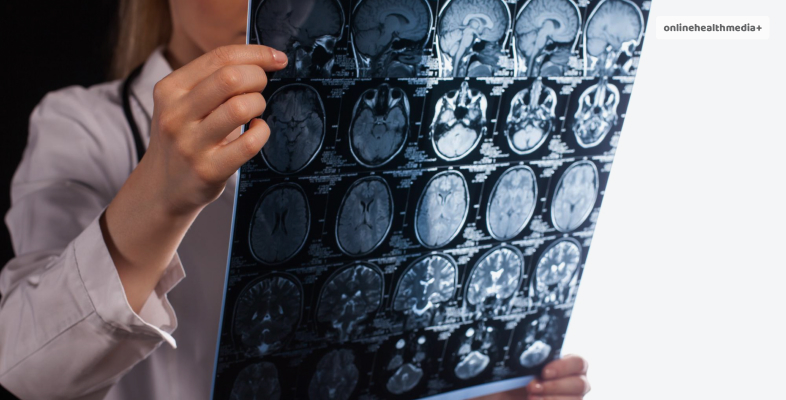
Answering the question “what is frontotemporal dementia” will require providing its definition. Frontotemporal dementia affects parts of the frontal and temporal lobes, making them shrink.
This is known as atrophy. Frontotemporal dementia can make people emotionally indifferent, socially inappropriate and impulsive. Others may even lose their ability to properly use language.
Frontotemporal dementia encompasses a group of related disorders that share common pathological features but present with different clinical symptoms.
The three main subtypes of FTD are behavioral variant frontotemporal dementia (bvFTD), primary progressive aphasia (PPA), and semantic variant primary progressive aphasia (svPPA).
Each subtype is characterized by distinct patterns of cognitive and behavioral symptoms:
- Behavioral Variant Frontotemporal Dementia (bvFTD): This subtype is characterized by changes in behavior, personality, and social cognition. Individuals with bvFTD may exhibit:
- Disinhibition,
- Impulsivity,
- Apathy,
- Social withdrawal,
- Lack of empathy,
- Repetitive behaviors, and
- Inappropriate social conduct.
Cognitive deficits may include executive dysfunction, poor judgment, and impaired insight into their own behavior.
- Primary Progressive Aphasia (PPA): PPA is a subtype of FTD characterized by progressive language impairment. Individuals with PPA may experience:
- Difficulties with speech production (Non-fluent/Agrammatic Variant PPA),
- Word-finding difficulties, and
- Comprehension deficits (semantic variant PPA), or both.
Unlike other forms of dementia where memory is typically affected early on, memory function remains relatively preserved in the early stages of PPA.
- Semantic Variant Primary Progressive Aphasia (svPPA): SvPPA is characterized by deficits in language comprehension and semantic memory. Individuals with svPPA may have:
- Difficulty understanding the meanings of words and concepts, as well as
- Naming objects and
- Recognizing familiar faces or objects.
This subtype is often associated with changes in social behavior and emotional regulation.
What Stage of Dementia is Sundowning?

“What is frontotemporal dementia” can also have a follow-up question where you’re asking about sundowning.
Sundowning, also known as “late-day confusion,” is a common phenomenon observed in individuals with dementia, including Alzheimer’s disease and certain types of FTD.
It refers to the onset or worsening of behavioral symptoms, such as agitation, confusion, restlessness, or aggression, during the late afternoon or evening hours.
While sundowning can occur in any stage of dementia, it is often more pronounced in the moderate to severe stages when cognitive impairment is more advanced.
What are the Early Signs of Dementia?

Recognizing the early signs of dementia is crucial for early detection and intervention. Common early signs of dementia may include:
1. Memory Loss: Difficulty remembering recent events, appointments, or conversations.
2. Difficulty with Language: Problems finding the right words, following conversations, or understanding instructions.
3. Changes in Mood or Behavior: Mood swings, irritability, apathy, withdrawal from social activities, or uncharacteristic aggression.
4. Impaired Judgment: Poor decision-making, impulsivity, or lack of insight into one’s own behavior.
5. Difficulty with Familiar Tasks: Challenges with tasks that were previously routine or automatic, such as cooking, driving, or managing finances.
6. Disorientation: Confusion about time, place, or identity.
7. Changes in Personality: Changes in behavior, personality, or social conduct, such as increased apathy, disinhibition, or socially inappropriate behavior.
What Causes Frontotemporal Dementia?

Frontotemporal dementia is caused by the progressive degeneration and loss of nerve cells in the frontal and temporal lobes of the brain.
The exact cause of FTD is not fully understood, but it is believed to result from a combination of genetic, environmental, and lifestyle factors.
Some cases of FTD are associated with specific genetic mutations, such as mutations in the C9orf72, MAPT, and GRN genes, which can be inherited in an autosomal dominant pattern.
Other cases may be sporadic or idiopathic, with no known genetic cause.
Risk Factors and Protective Factors:
Understanding the risk factors associated with the development of frontotemporal dementia (FTD) is essential for early detection and intervention.
While the exact cause of FTD is not fully understood, several factors may increase the risk of developing the condition.
These risk factors include genetic predisposition, age, environmental exposures, and certain medical conditions.
1. Genetic Predisposition: Individuals with a family history of FTD or specific genetic mutations associated with the condition are at an increased risk of developing FTD. Mutations in genes such as C9orf72, MAPT, and GRN have been linked to inherited forms of FTD, although not all cases of FTD are hereditary.
2. Age: While FTD can occur at any age, it is more commonly diagnosed in individuals between the ages of 40 and 65. However, late-onset cases of FTD can also occur in older adults.
3. Environmental Exposures: Exposure to certain environmental toxins or chemicals may increase the risk of developing FTD. While the specific environmental factors implicated in FTD remain unclear, research suggests that factors such as pesticide exposure or head trauma may play a role in disease pathogenesis.
4. Medical Conditions: Certain medical conditions, such as traumatic brain injury, frontotemporal lobar degeneration, or other neurodegenerative diseases, may predispose individuals to FTD. Additionally, individuals with a history of psychiatric disorders or mood disturbances may be at increased risk of developing FTD.
Protective factors against FTD
Conversely, several protective factors may help reduce the risk of developing FTD or delay the onset of symptoms. These protective factors include:
1. Healthy Lifestyle Habits: Adopting a healthy lifestyle, including regular physical exercise, a balanced diet, and mental stimulation, may help protect against cognitive decline and neurodegenerative diseases such as FTD. Engaging in activities that promote cognitive health, such as reading, puzzles, or social interactions, may help maintain brain function and resilience.
2. Social Engagement: Maintaining social connections and participating in meaningful activities can help support cognitive health and emotional well-being. Social engagement may help reduce feelings of isolation, depression, and anxiety, which are common risk factors for cognitive decline and dementia.
3. Education and Cognitive Reserve: Higher levels of education and cognitive stimulation have been associated with a reduced risk of developing dementia, including FTD. Building cognitive reserve through lifelong learning, challenging tasks, and intellectual pursuits may help protect against cognitive decline and delay the onset of symptoms in later life.
By understanding both the risk factors and protective factors associated with FTD, individuals and healthcare professionals can take proactive steps to mitigate risk factors and promote cognitive health and well-being.
What are the 7 Stages of Frontotemporal Dementia?

The progression of FTD varies from person to person, however, it’s division is often into seven stages based on the severity of symptoms and their impact on daily functioning. These stages may include:
1. Stage 1 (Preclinical Stage): In the preclinical stage, individuals may experience subtle changes in behavior, personality, or language that may not be apparent to others. Symptoms may include mild social disinhibition, language difficulties, or changes in mood or temperament.
2. Stage 2 (Early Stage): In the early stage, symptoms become more noticeable and may interfere with daily activities and social interactions. Individuals may exhibit changes in behavior, personality, or language, but they can still perform basic activities of daily living independently.
3. Stage 3 (Mild Stage): In the mild stage, cognitive and behavioral symptoms worsen, leading to greater impairment in social and occupational functioning. Individuals may have difficulty with language, executive function, and decision-making, requiring increased support and supervision.
4. Stage 4 (Moderate Stage): In the moderate stage, symptoms become more pronounced and may significantly impact daily functioning. Individuals may require assistance with activities of daily living, such as dressing, grooming, and meal preparation. Behavioral symptoms, such as impulsivity, apathy, or aggression, may also become more prominent.
5. Stage 5 (Moderate to Severe Stage): In the moderate to severe stage, cognitive and behavioral deficits continue to worsen, resulting in significant functional impairment. Individuals may have difficulty with communication, memory, and executive function, requiring extensive support and supervision from caregivers.
6. Stage 6 (Severe Stage): In the severe stage, individuals experience profound cognitive and functional decline, requiring round-the-clock care and assistance with all activities of daily living. Behavioral symptoms may be severe and challenging to manage, and individuals may be at increased risk of falls, infections, and other complications.
7. Stage 7 (End-stage): In the end-stage, individuals are completely dependent on others for all aspects of care. They may lose the ability to communicate verbally, move independently, or recognize familiar faces or objects. Quality of life may diminish greatly. Moreover, individuals may be at risk of complications such as aspiration pneumonia or pressure ulcers.
Diagnosis and Differential Diagnosis
Diagnosing frontotemporal dementia (FTD) requires a comprehensive evaluation by a healthcare professional, including a thorough medical history review, physical examination, cognitive assessments, laboratory tests, and brain imaging studies.
While there is no single test that can definitively diagnose FTD, a combination of assessments and evaluations is used to make an accurate diagnosis and differentiate FTD from other conditions that may present similar symptoms.
1. Specialized Assessments: Neuropsychological testing, functional imaging studies (e.g., functional MRI), and genetic testing may aid in the diagnosis of FTD. Additionally, they help differentiate it from other neurodegenerative disorders. Neuropsychological testing assesses various aspects of cognitive function, including memory, language, executive function, and visuospatial abilities, to identify patterns of cognitive impairment consistent with FTD.
2. Differential Diagnosis: It is essential to distinguish FTD from other conditions that may present with similar symptoms, such as Alzheimer’s disease, Parkinson’s disease, or psychiatric disorders. Differential diagnosis involves ruling out other potential causes of cognitive impairment through a thorough assessment of medical history, physical examination, laboratory tests, and brain imaging studies.
3. Clinical Criteria: The diagnosis of FTD is based on clinical criteria established by consensus guidelines, such as the International Consensus Criteria for Behavioral Variant FTD or the International Working Group criteria for Primary Progressive Aphasia. These criteria outline specific clinical features, neuropsychological findings, and imaging patterns that support a diagnosis of FTD and help differentiate it from other conditions.
4. Multidisciplinary Evaluation: Diagnosing FTD often requires a multidisciplinary approach involving collaboration between primary care physicians, neurologists, neuropsychologists, and other specialists. A comprehensive evaluation allows for a thorough assessment of cognitive, behavioral, and functional domains and ensures that individuals receive an accurate diagnosis and appropriate management plan.
Employing a systematic approach to diagnosis and considering the full range of clinical, and other findings, healthcare professionals can effectively diagnose FTD.
Moreover, they can differentiate it from other conditions. Moreover, leads to timely intervention and support for affected individuals and their families.
Treatment Options For Frontotemporal Dementia
The treatment of conditions such as dementia and its types become difficult due to this disorder. This is why scientists and researchers are still trying to find a cure for the condition.
The research so far has been successful in improving the diagnosis of the condition. However, it is still difficult for doctors to cure frontotemporal dementia or any other type of dementia.
The one way treatment proceeds in this case are treating the symptoms that a patient is experiencing. It is also important to note that Alzheimer’s medicine is not helpful in this condition, thus, it is best to not self-medicate.
Always seek medical assistance when you develop signs of frontotemporal dementia. You can also know more about the condition by asking your doctor “what is frontotemporal dementia?”
Here’s all the treatment options that take care of the symptoms someone with frontotemporal dementia experiences:
- Antipsychotics: Antipsychotic medicines like quetiapine or olanzapine help treat the behavioral symptoms of the condition. If you are a family member reading this article to support your family member with a diagnosis of FTD, be careful of the side effects that these medications can cause.
- Antidepressants: These can also be prescribed for taking care of the behavioral symptoms. Your doctor may prescribe sertraline (Zoloft), escitalopram (Lexapro), Selective serotonin reuptake inhibitors (SSRIs).
- Speech therapy: Therapy is an option for people who may be having trouble with language. Communication aids can help the patient in improving their speech, which is one of the focuses of speech therapy.
These handful options remain for people with frontotemporal dementia to improve their experience of the condition.
In addition, they are also enabled to seek support for their wellbeing and improvement of quality of life.
Conclusion
In conclusion, frontotemporal dementia is a complex and progressive neurological disorder characterized by changes in behavior, and executive function.
Recognizing the early signs of FTD, understanding its stages of progression, and knowing its causes can help individuals and their families. Thus, to better navigate the challenges associated with this condition.
Early diagnosis and intervention are crucial for optimizing outcomes and quality of life for those affected by frontotemporal dementia.
Ongoing research and advances in understanding FTD hold promise for improved diagnosis, treatment, and care in the future.
Call 1-866-507-7222 (toll-free) Monday through Friday from 9 a.m. – 5 p.m. ET if you or your loved one needs support.
Also read
- Tips Every Aspiring Nurse Should Know.
- 5 Tips to Take Care of Your Sensitive Skin.
- What Is Red Light Therapy & What Are Its Main Benefits?



